Care of teeth in people with intellectual disabilities

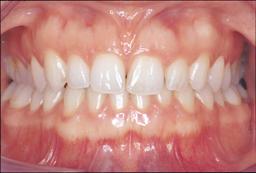 Healthy gums
Healthy gums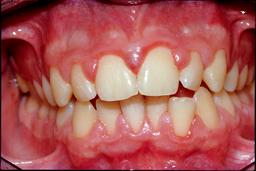 Inflamed gums
Inflamed gums
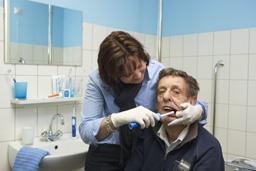
 Electric toothbrush
Electric toothbrush

 Use a non-abrasive toothpaste
Use a non-abrasive toothpaste

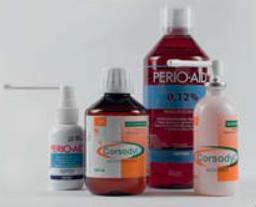 Rinses and mouth spray with chlorhexidine
Rinses and mouth spray with chlorhexidine
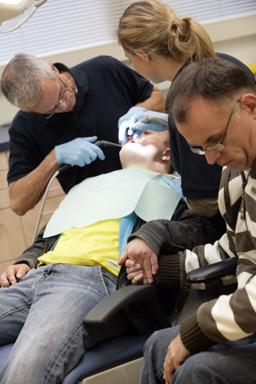
Everyone benefits from a healthy mouth. A healthy mouth allows you to eat and drink well. A fresh mouth also looks nice. People with intellectual disabilities are more likely to have problems in the mouth. Motor skills are often weak or completely limited. In the mouth, this manifests itself, for example, in weak lip, tongue and cheek muscles. But abnormal tooth position, muscle tension, damage to the teeth due to falling or bumping (epilepsy) or diet can also cause difficulties in the mouth. With good oral care, you can keep your child or client's teeth and gums healthy. Different ages have different oral problems. Whether you are brushing the teeth of a child or an adult with intellectual disabilities, you will encounter dilemmas to a greater or lesser extent. Here you can read about the most common problems and solutions for good oral care.
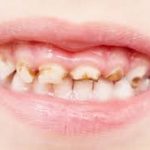
Dental plaque and cavities
Dental plaque is a white-yellow layer that is difficult to see. It forms on and between the teeth and on the transition to the gums. Plaque contains bacteria. These bacteria convert carbohydrates, such as sugar and starch from food and drinks, into acids in the mouth. These acids cause cavities (caries) in the teeth.
Plaque and inflamed gums
Healthy gums are pink, tight around the teeth and do not bleed when the teeth are brushed. Red, swollen or bleeding gums usually indicate inflamed gums. If you do not properly remove plaque on and between the teeth, the bacteria in the plaque cause the gums to become inflamed. Plaque that is not removed can harden and calcify into tartar. New plaque easily adheres to tartar. As a result, the gums become increasingly inflamed. The inflammation can even affect the underlying jawbone. Severe gum disease can lead to the loss of teeth.
Cavities and gum disease are infectious diseases with implications for both oral and general health.
How do you remove plaque?
Brushing teeth is the basis of good oral hygiene. It is a meticulous job and certainly not easy. For your child or client themselves, brushing teeth is probably too difficult. For that, your help is needed. But many children or clients quite often turn their heads away or push the brush away with their tongues. For example, they bite the brush, gag, have tight cheeks, lips and tongue, clamp the jaws together, have severe bleeding gums and pain reactions or otherwise resist. Good posture and the right tools will make brushing your child or client's teeth easier. Brush teeth carefully twice a day and not too vigorously. Use the brushing instructions for this. A good brushing takes two minutes. So take your time! Choose a time in the day when you can pay attention to oral care for your child or client, preferably in the morning after breakfast and in the evening before going to bed.
The Ivory Cross recommends brushing teeth twice a day for two minutes, but realises that this is not feasible in all situations. Brushing teeth carefully once a day is better than twice a day ‘half. Get other tips and advice for brushing your child's or client's teeth from your dentist or dental hygienist.
Choose a good toothbrush
Choose an electric toothbrush with a small brush head. When used properly, electric toothbrushes remove more plaque than manual toothbrushes. Brushing with an electric toothbrush definitely requires getting used to. Take two weeks to get used to it. Is it still not possible to brush electrically after this period? Then choose a manual toothbrush with soft bristles and a small brush head. Adult teeth can also be brushed with a child's brush, if this reduces resistance in your adult child or client. For all brushes, replace the toothbrush every three months or when the bristles start to stand apart.
Use fluoride toothpaste
Fluoride makes tooth enamel stronger and less soluble in acid. Therefore, use a toothpaste with fluoride. You can brush with fluoride toothpaste even if your child or client cannot rinse after brushing. Swallowing a little bit of toothpaste is no big deal. Sometimes it can be useful to brush without toothpaste. In that case, spread some fluoride toothpaste on the teeth with your finger after brushing. This way, you still apply fluoride to the teeth.
The basic fluoride recommendation reads:
- 0 and 1 year, from the breaking of the first teeth: brush once a day with fluoride toddler toothpaste
- 2, 3 and 4 years: brush twice a day with fluoride toddler toothpaste
- 5 years and above: brush twice a day with fluoride toothpaste
- For all ages: all other forms of fluoride use in consultation with dentist or dental hygienist
It is possible that your dentist or dental hygienist will recommend the use of extra fluoride for your child or client.
Use a toothpick or brush between teeth
A toothbrush alone cannot properly clean the spaces between the teeth. This applies to both a manual toothbrush and an electric toothbrush. Therefore, use a toothpick or a brush for the gaps. A good toothpick is made of wood, triangular in shape with a flat side and tapers to a point. They can vary in thickness. For larger gaps, you can use thicker sticks. For narrower gaps, choose a thinner variety. Brushes also come in all shapes and sizes. If possible, use a toothpick or brush once a day. Choose a convenient time, for example in the afternoon when it is a little quieter. Ask your dentist or dental hygienist which toothpick or brush is best for your child or client and ask for instructions. See also the instruction in this brochure.
And if polishing fails?
Sometimes it is not possible to use a toothbrush. A gauze or a finger toothbrush with fluoride toothpaste can be practical substitutes. If even this form of toothbrushing is not possible, a rinse or mouth spray based on chlorhexidine can help. This substance reduces the action of harmful bacteria in plaque. Before using it, always consult your dentist or dental hygienist and ask for instructions. This is because teeth may become discoloured by using a product containing chlorhexidine.
To the dentist or dental hygienist
Take your child or client to the dentist or dental hygienist at least twice a year. The teeth will then be properly checked and you will receive guidance on how to keep the mouth healthy. Invasive treatments can thus be avoided. Is there any pain? Don't put off a visit any longer and make an appointment. The dentist or dental hygienist may also suggest increasing the frequency of visits for your child or client. Not all dentists are experienced in treating people with disabilities. For example, they will refer to a colleague or to a Centre for Special Dentistry. You can get in touch with such a centre through the Association for the Promotion of Dental Health Care for the Disabled (VBTGG) and the Central Consultation on Special Dentistry (Cobijt). You will need a referral letter from your home dentist
Instruction on correct brushing posture in people with intellectual disabilities
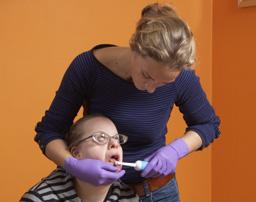 Get behind your child or client
Get behind your child or client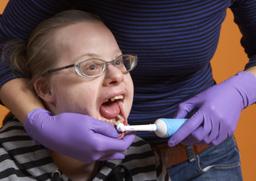 Fix the head
Fix the head Make the teeth visible with your hand
Make the teeth visible with your hand Oral check
Oral check
Proper brushing postureProper brushing posture is more important than you may think. Too often, parents or guardians stand in front of their child or client. But then you have little view into the mouth, you have no control over your child or client and you yourself are in a vulnerable position. Have your child or client sit and stand diagonally behind them. Fix the head and look into the mouth to see what you are doing. Press the cheek to the side with your finger in your child or client's mouth and push the lip away with your thumb.
Is your child or client lying down? If so, choose his or her preferred position. For example, raise the head slightly using a rolled-up towel on his or her neck. In children and clients with swallowing disorders, brushing teeth can increase the risk of choking. Brushing teeth can also trigger a gag reflex. Brush their teeth once without toothpaste. After brushing, apply a little fluoride toothpaste on your finger and ‘lubricate’ the teeth with it. Use a (electric) toothbrush and a toothpick or brush. Companions of clients are advised to wear gloves for hygiene reasons.
Opening the mouth
If your child or client will not or cannot open their mouth, provide mouth control. Bend the head slightly forward. This makes the mouth relax more easily. There are two ways: mouth control from the front (see photo) and from the side.
Mouth control from the front: Place your thumb of your left hand (for left-handers, the other hand) on the pad of the chin, your index finger on the cheek and your middle finger under the chin. Make sure your thumb does not touch the lower lip. Gently press on the cushion of the chin with your front thumb and upwards with your middle finger. The mouth opens.
Mouth control from the side: Place your index and middle finger of your left hand (for left-handers, the other hand) around the chin. Place your index finger on the pad of the chin, your middle finger stretched under it. Make sure your index finger does not touch the lower lip. Your thumb rests on your hand, not on the face. Press gently with your index finger on the pad of the chin and gently upwards with your middle finger. The mouth opens. Ask your dentist or dental hygienist for a demonstration.
Bite marks
If keeping the mouth open is very difficult, bite bits and blocks like those used by the dentist can sometimes help. There are bite bits and blocks (made of rubber and) of steamed beech wood. These do not produce sharp splinters, even when chewed to pieces. You can get them from your dentist or dental hygienist. You can also ask them for advice on how to use them.
Click here for an instruction on electric brushing.
Click here for an instruction on manual tooth brushing.
Click here For a toothpick instruction.
Click here for an instruction of the rager.
Oral problems in people with intellectual disabilities


 Let your child drink from a cup from 9 months onwards
Let your child drink from a cup from 9 months onwards





 Choose sugar-free chewing gum
Choose sugar-free chewing gum





People with intellectual disabilities are more likely to have gum disease and tooth decay (cavities). This has a number of causes:
Nutrition
Because of chewing and swallowing problems, people with intellectual disabilities often eat liquid, pureed or finely chopped, soft (tube) food. They also often keep food in the mouth for a long time. Soft food reduces the mouth's natural self-cleaning ability. Consumption of soft (tube) food encourages plaque formation. Once plaque hardens, it becomes tartar. New plaque easily ‘sticks’ to tartar.
What to do with soft food
Oral hygiene is the key word here. Make sure you remove all plaque daily to prevent cavities and gum disease.
Reduced natural cleaning of the mouth
Not only soft foods cause reduced self-cleaning of the mouth. Rigid and flaccid paralyses of the mouth muscles, constant holding of the mouth open and mouth breathing are also causes of reduced natural cleaning of the mouth.
What to do when natural mouth cleansing is impaired
Oral hygiene applies here too. Make sure you remove all plaque daily to prevent cavities and gum disease.
Sucking or mouthing
Frequent sucking on a feeding bottle or anti-drip cup with sweet contents, for example fruit juice, syrup, drinking yoghurt and other milk products, can damage the teeth. Because the teeth are in contact with sugars for long periods of time, there is a high risk of developing so-called infant caries.
What to do when sucking or mouthing
Limit sweet drinks. Alternatively, give water or plain tea without sugar if possible. Let your child or client drink sweet drinks in one sitting. If possible, use an ordinary cup, e.g. with a straw. In the evening and at night, drinking from a feeding bottle with sweet contents is especially harmful. At night, the saliva can hardly recover the acid attacks on the teeth. Drinking water (at night) from a baby bottle is not harmful, by the way.
Reflux and rumination of food
Stomach acid is extremely acidic. Acids that enter the mouth attack tooth enamel. This form of irreparable tooth wear is called tooth erosion. Some clients return stomach contents to the mouth (rumination or rumination) or suffer from spontaneous return of food (reflux). In reflux, stomach acid flows back down the oesophagus into the oral cavity due to a malfunction of the sphincter between the oesophagus and stomach.
What to do in case of reflux or rumination
Acid-inhibiting drugs may help. Sometimes reflux surgery may be necessary. Dietary modification may also have an effect. For dietary advice, contact the dietician(s).
Disorder in the change order
Children are usually born toothless. A child changes its milk teeth between the ages of six and 12. At least, that is how it is written in ‘the books’. With your child or client, the changeover period may be different. Children with intellectual disabilities often have small jaws. As a result, the teeth do not fit in. Often, a child does not change all his teeth, but partially, while the permanent teeth are in place. The timing of the teeth coming through may also differ.
What to do when switching
The enamel of newly erupted teeth is still very porous and vulnerable. Brush the tips of new teeth as soon as they have erupted. When new teeth emerge, the gums often swell. This is normal. It can be painful, but you need not worry. Visit your dentist regularly for check-ups.
Deviant tooth position
Many people with intellectual disabilities have abnormalities in the position, shape and number of teeth. If teeth are neatly lined up, you can clean them well. It becomes much more difficult if they are crooked or one behind the other, for example. It is difficult to reach them with the brush. A deviated tooth position usually has no consequences for the health of teeth.
What to do in case of an abnormal tooth position
Extra attention to oral hygiene. Pay particular attention to the spaces between teeth. Sometimes the dentist can improve an abnormal tooth position with braces or, for example, implants. The dentist may also recommend shortening the dental arch (extracting molars) to make brushing teeth easier.
Use of medicines
Several drugs have the side effect of inhibiting the salivary glands from releasing saliva. These are mainly drugs used in the treatment of high blood pressure (antihypertensives), cardiac arrhythmias (digoxin, anti-arrhythmics) or medications, such as antidepressants, sleep aids and urinals. The drugs usually do not affect the salivary glands themselves, but only inhibit salivary flow. Saliva has a lubricating effect on speaking, chewing and swallowing. Saliva helps us move our cheeks, tongue and lips more easily. With saliva, we moisten our food in such a way that we can swallow it painlessly. Saliva also moisturises the oral mucosa, preventing dehydration. Moreover, it has a cleansing effect on teeth, molars and the oral mucosa. In addition, saliva inhibits the action and growth of bacteria and fungi in the mouth, preventing mouth infections. If your child or client does not have enough saliva, plaque forms faster than normal. This causes cavities to form more quickly. This happens especially if your child or client regularly eats or drinks sugary foods. In a dry mouth, plaque formation and cavities occur mainly along the edges of the gums. This can also cause the gums to become inflamed. Taking medication can also have other consequences, such as gum growth (anti-epilepsy drugs), discolouration of the teeth (chlorhexidine) and the production of too much saliva, i.e. drooling (analgesics, antipsychotics, anti-stroke drugs).
What to do in case of dry mouth
AIf medicine use is the cause of your child's or client's dry mouth, discuss with the GP or specialist whether you can adjust the type of medicine, dosage or time of administration. You can stimulate your child or client's speech production by giving them food they need to chew well. Think firm brown sandwiches, carrots or sugar-free chewing gum. The release of saliva can also be enhanced by eating slightly acidic foods, such as fruit or cucumber. This often does not work, or works insufficiently, in people who have suffered from Sjögren's syndrome for some time or who have had radiation in the head or neck.
What to do in case of gum growth
Tell the dentist or dental hygienist that your child or client has started medication. Right from the start, extra good oral hygiene is important. Then you can prevent gum growth in your child or client. This is because gums grow mainly in places where there is plaque. Removing that plaque is therefore extra important. Especially as brushing away plaque in those places becomes increasingly difficult. Red, swollen and bleeding gums are inflamed. Inflammation never goes away by itself. Good oral hygiene is extra important. Visit the dentist or dental hygienist regularly to have your child's or client's mouth cleaned.
What to do in case of drooling
Eating sugary foods increases saliva production. Therefore, give your child or client as little of it as possible. Close your child or client's mouth as much as possible. If symptoms persist, contact your GP, dentist or speech therapist.
Dental injury
Children and adults with epilepsy may fall at an unexpected time. Someone who falls on their face is at risk of breaking or losing their teeth. People who have poor mobility, or are otherwise motor impaired, often walk more unsteadily and are therefore more likely to suffer dental injuries. Then there is a group of patients who damage themselves. They suffer from self-mutilation. Automutilation can lead to dental injury.
What to do in case of tooth injury
If the tooth is chipped, loose or out of the mouth: go to the dentist immediately. Keep (the chipped part of) the tooth wet in milk.
Habits
Thumbing in a mouth with permanent teeth is bad for tooth position. Sucking on cloths, teats and fingers can also lead to abnormal tooth position. People with intellectual disabilities often suck extremely, changing the tooth position. An abnormal tooth position can make oral hygiene more difficult. However, nail biting and teeth grinding (bruxism) also increase the risk of tooth wear.
What to do about bad habits
Try to unlearn the deviant habits in your child or client. Encourage positive behaviour. Seek advice from your dentist, dental hygienist, speech therapist or remedial therapist.
Down syndrome
People with Down syndrome often have weak tongue and mouth muscles. These make it difficult to swallow, eat, drink and speak. As a result, the mouth's self-cleaning function does not work as well. More plaque is the result. People with Down breathe more through the mouth. A dry mouth is then the result. As a result, the protective effect of saliva is limited. Due to the reduced resistance, these people are more likely to contract serious (gum) infections. Moreover, the roots of the teeth of people with Down are often short. In case of gum inflammation, they are therefore more likely to become loose.
What to do in Down syndrome
Promote good oral habits. Teach your child or client to keep the tongue in the right place as much as possible, i.e. as much as possible behind the front teeth. Start this early. Proper use of the tongue is encouraged more by breastfeeding than by bottle feeding. A speech therapist can explain how to use the tongue properly and give you exercises. Try to encourage your child or client to breathe through the nose. You can do this by consistently closing the mouth when your child or client is sleeping.
Cleaning of prostheses and implants in people with intellectual disabilities
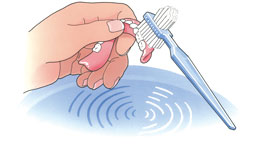
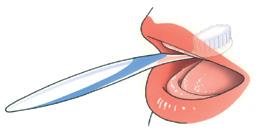
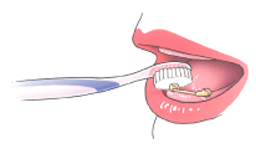
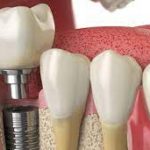
Many adults with intellectual disabilities wear dentures (false teeth). Nowadays, implant treatment is also possible for people with intellectual disabilities. An implant is a kind of artificial root that is screwed into the jaw onto which the dentist can attach a crown (tooth or molar), bridge (more teeth or molars) or prosthesis (dentures). In both situations, good oral hygiene is very important to prevent infection and inflammation.
Cleaning the prosthesis
Your client's dentures, like their own teeth, should be cleaned thoroughly every day. If you do not clean the dentures regularly, food residue will remain. Both on the dentures and underneath them. If you do not remove them, the gums may become inflamed. Preferably rinse the denture and mouth with water after every meal. Remove food particles on the denture and in the mouth. Use a special denture brush, e.g. from Lactona or Oral-B, to brush the denture thoroughly to remove plaque. Do not use toothpaste. It can be too abrasive. Use water and a mild liquid soap. Clean dentures always feel smooth. Do not let the smooth dentures slip out of your hands during cleaning. It will break. To be safe, fill the sink with water first and clean the dentures above it.
Once a week, put the dentures in vinegar overnight. This will prevent tartar from forming on the dentures. Afterwards, brush the dentures well and rinse them with water. Never put the dentures in hot water and definitely do not use bleach or abrasives. If necessary, ask your client's practitioner for advice.
Also clean your client's mouth
Besides the denture, clean the mucous membrane on which the denture rests: the jaws, the palate and the transition from the jaw to the cheeks. Otherwise, nasty infections can occur. And again, prevention is better than cure. Massage the mucous membrane at least once a day with a soft toothbrush and water. Pay extra attention to the palate. Start at the front of the mouth and let your child/client get used to you brushing their mouth. Always start on the outside in the lower jaw. This is the easiest area for your child or client to get used to and causes the least resistance. Move the brush up a little each time. Then brush the inside of the lower jaw. Then brush the outside of the upper jaw, followed by the inside of the upper jaw. If your child or client gags easily, it is best to brush from the middle to the side and back. See proper brushing posture and methods of opening the mouth elsewhere in this brochure.
Take off dentures at night
’At night, you should leave the denture out of your child or client's mouth to keep the mucosa on which the denture rests healthy. After cleaning, keep the denture in a container of clean water. Brush the denture again in the morning before replacing it in your child or client's mouth.
Denture cleaners
There are several denture cleansers on the market. The hydrogen peroxide in them has an antibacterial effect. A cleanser inhibits or removes discolouration from coffee, tea, wine and tobacco, among others, and is refreshing. A cleanser does not dissolve plaque. For this, brushing is necessary. Excessive use of these cleansers can damage the denture. The denture may fade and the surface may become rougher. For your child or client, denture cleaning tablets can be life-threatening. Damage to the oesophagus may also occur if your child or client mistakes the tablet for a sweet. It is therefore recommended to use water and liquid soap daily and vinegar once a week.
Cleaning implants
An implant under a crown or bridge is anchored in the bone. It is very important to properly clean the transition from the crown or bridge to the gums. Brush this area carefully with a soft (electric) toothbrush with fluoride toothpaste, using toothpicks or interdental brushes. Oral hygiene is very important with implants, also for people with disabilities. With poor oral hygiene, your child or client may lose their implant.
Implants that serve as pillars under overdentures should be cleaned with a soft toothbrush and toothpaste, brushes and/or (super)floss. Brush the part of the implant that protrudes above the gums twice a day. Pay special attention to the transition from the implant to the gums. Clean the area under the splint with brushes and/or super floss as directed by the dentist or dental hygienist. As directed by the dentist or dental hygienist, you can apply chlorhexidine gel around the implant once a day and place the denture over it.
If you do not remove food debris and plaque around the implants, the gums will become inflamed. As a result, they eventually lose their hold, become loose and can cause pain. Also check out proper brushing posture, methods of opening the mouth and brushing instructions.
For more information on oral and dental problems, oral care and oral health for people with intellectual disabilities, please visit or visit:
- Association for the Promotion of Dental Health Care for the Disabled (VBTGG) provides information on dental care foro people with disabilities.
- Central Consultation Special Dentistry (COBIJT) lists the centres for special dentistry established in the Netherlands.
- Dutch Society for Children's Dentistry (NVvK) lists the paediatric dentists working in the Netherlands.
- The Dutch Association for Speech Therapy and Phoniatrics (NVLF). The website informs about the work of the speech therapist: developing and, where necessary, restoring oral functions. Disorders
in the mouth can arise from neurological disorders or diseases. - LFB is an interest group by people with intellectual disabilities that advocates for the interests of people with intellectual disabilities.
- Kiesbeter.co.uk is a public healthcare portal intended for all adult residents of the Netherlands who have questions about care, health insurance and health. Disability care in the Netherlands can be searched and compared based on care, services and accommodation provided. The site also offers general information on disability care.
Want to know more?
Then download the free GezondeMond app. The app is available for Android and tablets, available via Google Play. The app for iPhone and iPad can be found in the iTunes App Store..


<< Back© Ivory Cross